What Is Malaria?

Malaria is a life-threatening disease caused by tiny parasites called Plasmodium, spread through the bite of an infected female Anopheles mosquito. Even though it’s preventable and treatable, malaria still affects millions of people every year, especially in tropical countries.
People usually first hear about malaria with a mix of confusion and worry — Can it spread easily? Is it very dangerous? How do I know if I have it?
This is normal. Malaria can be scary because symptoms often start like the common flu, but the disease can progress quickly if ignored.
What makes malaria important is that:
- It spreads silently through mosquito bites.
- Anyone can get it, regardless of age or gender.
- Early treatment can save lives and prevent complications.
At its core, malaria is simply an infection caused by parasites entering the bloodstream, multiplying inside the body, and causing fever, chills, and weakness. Understanding it clearly helps people protect themselves and seek help at the right time.
How Malaria Spreads (Transmission)
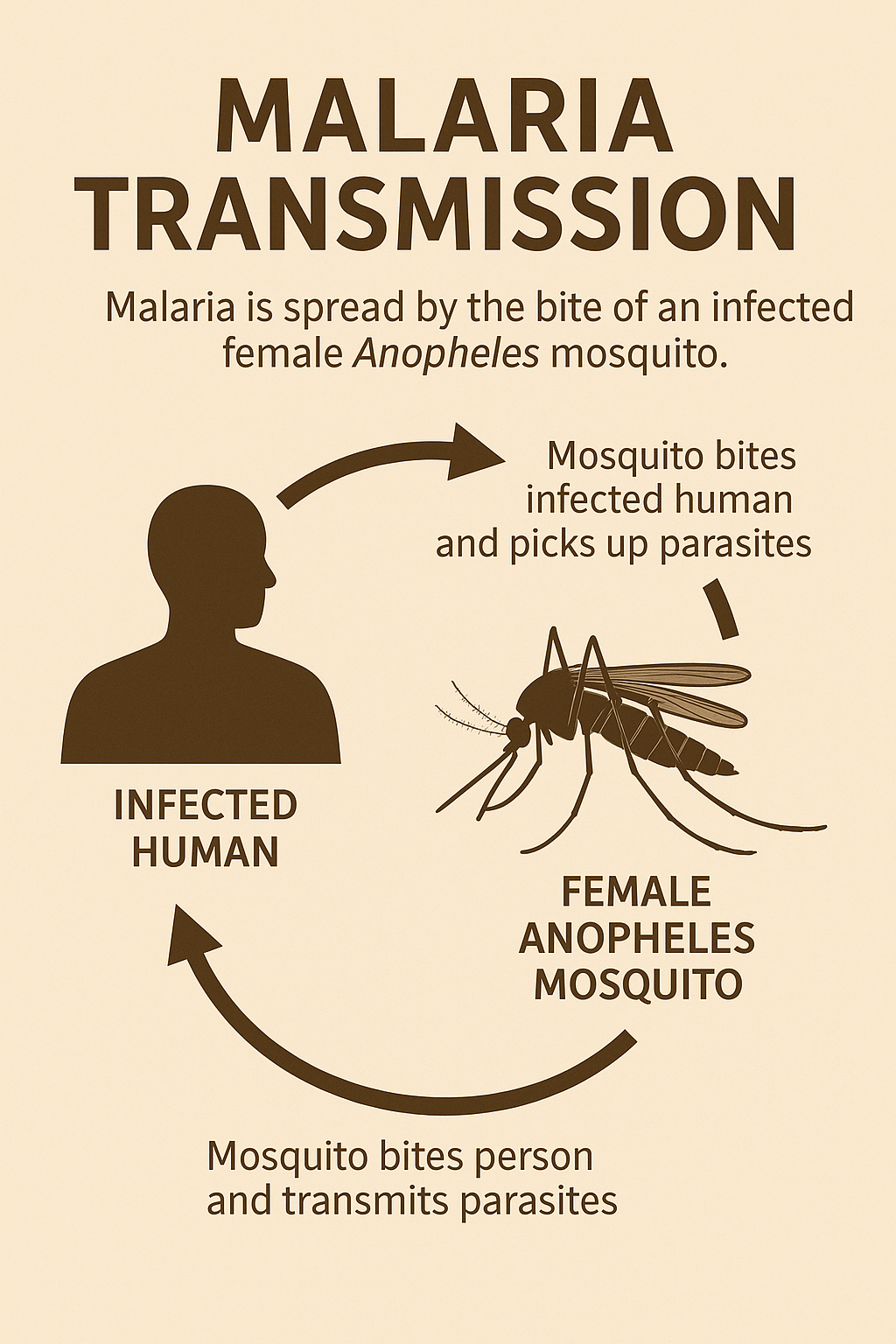
Malaria doesn’t spread from person to person like a cold. It needs a specific mosquito — the female Anopheles mosquito — to carry the parasite. Understanding this gives people more control and less fear because they know exactly how infection happens.
Here’s the simple chain:
1. Infected mosquito bites a person
When an Anopheles mosquito carrying Plasmodium parasites bites someone, it injects the parasite into their bloodstream.
2. Parasites travel to the liver
Once inside the body, these parasites quietly move to the liver, multiply, and get ready to infect red blood cells.
3. They enter red blood cells and multiply rapidly
This is when symptoms start — fever, chills, weakness — because infected RBCs burst, releasing more parasites.
4. A new mosquito bites this infected person
If another mosquito bites this person, it picks up the parasites and becomes infected.
5. That mosquito spreads malaria to others
And the cycle continues.
Important Things Readers Want to Know
- Only female Anopheles mosquitoes spread malaria.
They bite mostly at night or early morning. - You CANNOT get malaria through touching, sharing food, or talking.
- Stagnant water increases mosquito breeding, which increases risk.
- Blood transfusions and contaminated needles can rarely transmit malaria, but mosquito bites remain the main cause.
In short, malaria spreads through a simple mosquito–human–mosquito cycle. Breaking this cycle through prevention — nets, sprays, cleaning stagnant water — can dramatically reduce the risk..
Causes: The Plasmodium Parasites
Malaria isn’t caused by mosquitoes directly — it’s caused by parasites called Plasmodium. The mosquito is simply the carrier. These parasites are incredibly small, but once they enter the bloodstream, they can make a person very sick.
The Five Plasmodium Species That Infect Humans
Each species behaves differently, and knowing them helps people understand why malaria can be mild in some cases and severe in others.
1. Plasmodium falciparum
The most dangerous and the most common in India and Africa.
It multiplies very fast and can lead to severe malaria, organ failure, and cerebral malaria if not treated quickly.
2. Plasmodium vivax
Very common in Asia, including India.
It can stay dormant in the liver and reactivate weeks or months later, causing repeated episodes.
3. Plasmodium malariae
Causes a slower, milder form of malaria but can lead to long-term infection if untreated.
4. Plasmodium ovale
Less common. Similar to P. vivax, it can also hide in the liver and reappear later.
5. Plasmodium knowlesi
Originally found in monkeys, but now infects humans in some parts of Southeast Asia.
It can progress rapidly, so early diagnosis is important.
How the Parasite Actually Causes Illness
Once inside the body, these parasites:
- Enter the liver and multiply
- Move into red blood cells
- Break them open again and again
- Release toxins that cause fever, chills, weakness, and complications
This constant destruction of red blood cells is what makes malaria dangerous.
In short, the real “cause” of malaria is the Plasmodium parasite, and the mosquito is just the vehicle that helps it spread.
Signs and Symptoms of Malaria
Malaria can feel confusing in the beginning because its early symptoms look very similar to a normal viral fever. Many people ignore it for a day or two, thinking it’s just tiredness or seasonal illness. But malaria has a pattern and a progression that sets it apart.
Early Symptoms (Common and Often Mild at First)
These start when the parasite begins destroying red blood cells.
- Fever (comes and goes)
- Chills and shivering
- Headache
- Body ache or joint pain
- Weakness and fatigue
- Sweating after fever breaks
- Nausea or vomiting
These symptoms can appear 10–15 days after the mosquito bite.
Classic Malaria Fever Pattern
Many patients experience a cycle:
- Cold stage – intense chills, shivering
- Hot stage – high fever, warm skin, headache
- Sweating stage – fever drops, sweating starts, person feels exhausted
Not everyone gets this exact pattern, but when it happens, it’s a strong sign of malaria.
Symptoms of Severe Malaria (Red Flags)
These appear when the infection becomes dangerous and needs urgent treatment.
- Very high fever
- Confusion or altered consciousness
- Severe anemia
- Shortness of breath
- Seizures
- Jaundice (yellow eyes/skin)
- Dark or reduced urine
- Organ failure signs (kidney, liver)
If any of these appear, the person should get medical care immediately — severe malaria can progress quickly.
Why Recognizing Symptoms Early Matters
Early symptoms might seem small, but catching malaria early:
- Prevents complications
- Reduces hospitalisation
- Helps treatment work faster
- Protects others from getting infected (by breaking the mosquito cycle)
Types of Malaria
Malaria isn’t the same in every person. The type depends on how severe the infection is and which Plasmodium parasite is involved. Understanding this helps people recognise risk levels and know when to seek faster medical care.
A. Uncomplicated Malaria
This is the milder and more common form.
Symptoms are uncomfortable but not life-threatening when treated early.
Key features:
- Fever, chills, headache
- Sweating after fever
- Body ache and weakness
- Normal mental state (no confusion)
- No organ damage
With proper diagnosis and medicines, people usually recover well.
B. Severe Malaria
This is the dangerous form and needs urgent treatment in a hospital.
It is commonly caused by Plasmodium falciparum, the most deadly species.
Warning features include:
- Extremely high fever
- Severe anemia
- Breathing difficulty
- Confusion, seizures, or coma (cerebral malaria)
- Jaundice
- Kidney or liver failure
- Shock or very low blood pressure
Severe malaria can progress fast, so early detection is lifesaving.
C. Species-Based Types
Readers often want to know how malaria differs by parasite type:
- Falciparum malaria – most severe, fast progression
- Vivax malaria – causes relapses because it hides in the liver
- Malariae malaria – slow, long-lasting infections
- Ovale malaria – rare, can relapse like vivax
- Knowlesi malaria – rapid progression, found in Southeast Asia
Each species behaves differently, which is why proper diagnosis is essential.
Why Knowing the Type Matters
- Guides the doctor in choosing the right treatment
- Helps predict whether the infection might relapse
- Identifies emergency cases early
- Helps families understand seriousness and take precautions
Diagnosis of Malaria
When someone has fever that keeps coming back, chills, or weakness, the biggest question in their mind is:
“Is this malaria or just a viral fever?”
Diagnosis removes that uncertainty. It confirms the infection early, guides the right treatment, and prevents complications. Thankfully, malaria tests are quick, accurate, and easily available.
1. Blood Smear Test (Gold Standard)
This is the most commonly used and reliable test.
- A small drop of blood is checked under a microscope.
- It shows whether malaria parasites are present.
- It also identifies the species (falciparum, vivax, etc.)
- And tells how many parasites are in the blood (parasite count).
Doctors trust this test because it gives detailed, accurate results.
2. Rapid Diagnostic Tests (RDTs)
These are simple “strip tests” that give results in 15–20 minutes.
- Useful in clinics, villages, and emergency situations.
- Detects malaria antigens in the blood.
- Helps quickly confirm falciparum or vivax infection.
It’s fast, easy, and ideal when a microscope isn’t available.
3. Full Blood Count (CBC) (Supportive Test)
CBC doesn’t diagnose malaria directly, but it shows important changes:
- Low hemoglobin (anemia)
- Low platelets
- High or low WBC count
These patterns often support the diagnosis and show severity.
4. Polymerase Chain Reaction (PCR) – Advanced Test
Used rarely in routine cases because it is expensive and slow.
But it’s extremely accurate and used for:
- Research
- Complicated cases
- Mixed-species infections
- Confirming doubtful results
When Should a Person Get Tested?
Testing is important if someone has:
- Fever with chills
- Fever that repeats every 1–2 days
- Headache and body pain
- Recent travel to a malaria-prone area
- Symptoms of severe malaria (confusion, breathlessness, jaundice)
Early testing means early treatment — and that changes everything.
Treatment Options for Malaria
Hearing the word malaria can make people anxious, but the reassuring truth is this: malaria is treatable, especially when diagnosed early. Treatment works best when the exact species of parasite is known, because different types respond to different medicines.
The goal of treatment is simple — kill the parasites, control symptoms, and prevent complications.
1. Antimalarial Medicines (Main Treatment)
Doctors choose medicines based on the type of malaria:
A. Artemisinin-based Combination Therapy (ACT)
This is the first-line treatment for Plasmodium falciparum (the most dangerous type).
Examples include:
- Artemether–Lumefantrine
- Artesunate–Amodiaquine
- Artesunate–Mefloquine
Benefits:
- Works fast
- Clears parasites quickly
- Reduces the risk of severe malaria
B. Chloroquine
Used for P. vivax, P. malariae, or P. ovale in regions where resistance is low.
C. Primaquine
Very important for P. vivax and P. ovale because these species hide in the liver and cause relapses.
Primaquine clears these hidden parasites, preventing future attacks.
(Note: G6PD test is required before starting primaquine.)
2. Treatment for Severe Malaria (Emergency Care)
Severe malaria needs hospital management.
The preferred drug is:
- Injectable Artesunate
If Artesunate isn’t available, doctors may use:
- Quinidine or Quinine (less preferred)
Along with this, supportive care is provided:
- IV fluids
- Oxygen
- Blood transfusion (if anemia is severe)
- Treatment for seizures or organ failure
3. Supportive Treatment
Readers often want to know how to feel better during recovery:
- Plenty of fluids to prevent dehydration
- Fever control with paracetamol
- Nutritious, light meals
- Rest until the fever cycle stops
4. Why Completing the Full Course Is Crucial
Stopping treatment early can:
- Cause malaria to return
- Increase chances of resistance
- Make the infection harder to cure later
Finishing all doses ensures the parasite is fully cleared.
In Simple Words
Malaria treatment is effective, available, and life-saving.
Early diagnosis + correct medicine = fast recovery and fewer complications.
Complications of Malaria
Malaria can start like a simple fever, but if it isn’t treated on time, it can quickly turn dangerous. These complications happen because the parasite destroys red blood cells, affects organs, and reduces oxygen supply in the body.
1. Cerebral Malaria (Brain Involvement)
This is one of the most serious complications caused mainly by Plasmodium falciparum.
Symptoms:
- Confusion
- Seizures
- Loss of consciousness
- Coma
It can be life-threatening and requires immediate hospital care.
2. Severe Anemia
Malaria destroys red blood cells at a fast rate.
This leads to:
- Extreme tiredness
- Pale skin
- Shortness of breath
- Weakness
Children and pregnant women are especially at risk.
3. Kidney Failure
The kidneys may stop working properly due to dehydration, destruction of red blood cells, and toxins.
Signs include:
- Reduced urine
- Swelling
- Fluid retention
This may require dialysis in severe cases.
4. Liver Failure and Jaundice
The liver becomes overloaded while clearing parasites.
Signs:
- Yellow eyes and skin
- Dark urine
- Vomiting
- Severe weakness
5. Breathing Problems (Respiratory Distress)
Fluid can build up in the lungs or the body becomes too acidic.
This causes:
- Difficulty breathing
- Fast breathing
- Low oxygen levels
It’s a medical emergency.
6. Low Blood Sugar (Hypoglycemia)
Common in:
- Children
- Pregnant women
- Patients treated with quinine
Symptoms: sweating, shaking, confusion.
7. Shock (Very Low Blood Pressure)
Happens when the body can’t maintain blood flow properly.
This can lead to organ failure if not treated quickly.
8. Malaria in Pregnancy – Special Complications
Pregnant women have higher risk.
Complications include:
- Severe anemia
- Low birth weight baby
- Premature delivery
- Miscarriage (in severe infections)
Why Readers Must Understand This
Complications usually happen when:
- Malaria is ignored
- Symptoms are mistaken for viral fever
- Treatment is delayed
- The infection is caused by P. falciparum
Early testing + early treatment = prevents almost all complications.
Prevention Measures

Malaria prevention is all about breaking the mosquito–human–mosquito cycle. The more effectively we avoid mosquito bites and reduce breeding areas, the lower the chances of infection. Prevention gives people confidence because it turns fear into control.
Let’s break it down into practical steps that anyone can follow.
1. Use Mosquito Nets (Especially at Night)
Female Anopheles mosquitoes bite mostly at night.
Sleeping under long-lasting insecticidal nets (LLINs) reduces bites sharply.
Benefits:
- Affordable
- Safe for children and pregnant women
- Offers all-night protection
2. Apply Mosquito Repellents
Repellents create a protective layer on the skin.
Common options:
- DEET-based creams
- Picaridin
- Lemon-eucalyptus oil (natural option)
Apply especially in the evening and early morning.
3. Wear Protective Clothing
Long sleeves and long pants reduce skin exposure.
Light-colored clothing is better because it attracts fewer mosquitoes.
4. Keep Your Surroundings Clean
Mosquitoes breed in stagnant water.
Removing these breeding spots makes a huge difference.
Check weekly for:
- Buckets, flower pots
- Coolers
- Tyres
- Water tanks
- Open drains
- Garbage that holds water
Add larvicides where water cannot be emptied.
5. Use Indoor Residual Spraying (IRS)
Government health teams often spray insecticides inside walls.
This kills mosquitoes that rest indoors and lowers transmission in the area.
6. Window and Door Screens
Nets or mesh on windows and doors prevent mosquitoes from entering rooms.
7. Preventive Medicines for High-Risk Groups
Doctors may prescribe antimalarial tablets for:
- Travelers going to malaria-prone regions
- People living in high-transmission areas
- Pregnant women in certain high-risk zones (as per local guidelines)
This is called chemoprophylaxis.
8. Community-Level Prevention
Malaria control becomes stronger when the whole community participates:
- Fogging in outbreak areas
- Cleaning public spaces
- Awareness drives
- Reporting suspected cases early
Why Prevention Matters
- It protects families before malaria even starts.
- Reduces the number of mosquitoes in the area.
- Lowers hospital visits and complications.
- Helps control malaria at the community and national level.
High-Risk Groups
While malaria can affect anyone, certain groups are more vulnerable because their immune system is weaker or their exposure is higher. These groups need faster testing, stronger prevention, and careful monitoring.
1. Children Under 5 Years
Small children have an immature immune system.
So malaria can worsen quickly and lead to:
- Severe anemia
- Dehydration
- Seizures
- High fever spikes
Early treatment is critical for them.
2. Pregnant Women
Pregnancy naturally lowers immunity.
Risks include:
- Severe malaria
- Anemia
- Complications for the baby (low birth weight, premature birth)
They must use nets and repellents consistently.
3. Older Adults (Elderly)
Age reduces the body’s ability to fight infections.
Complications may develop faster, especially in those with other illnesses like diabetes or hypertension.
4. People With Weak Immune Systems
Includes individuals with:
- Chronic illnesses
- HIV/AIDS
- Nutritional deficiencies
They may not show typical symptoms at first, but the disease can become severe quickly.
5. Travelers Visiting High-Risk Areas
People who travel from malaria-free regions to tropical areas do not have natural immunity.
They are at high risk of sudden, severe infection.
Doctors often prescribe preventive medicines for them.
6. People Living in High-Transmission Zones
Regions with many mosquitoes and poor sanitation see repeated malaria cases.
These communities are more exposed and need strong environmental control.
Why Identifying High-Risk Groups Matters
- Helps focus prevention and early testing
- Reduces severe malaria cases
- Protects vulnerable populations
- Guides doctors on who needs urgent care
Malaria Control Programs in India
India has been working actively for years to reduce malaria cases and protect communities. These government programs combine early diagnosis, treatment, prevention, and public awareness. Knowing about these initiatives helps people trust the system and use services available to them.
1. National Vector Borne Disease Control Programme (NVBDCP)
This is the main national program responsible for controlling malaria and other mosquito-borne diseases.
Key focus areas:
- Early detection and prompt treatment
- Reducing mosquito breeding
- Indoor spraying with insecticides
- Providing mosquito nets
- Community awareness activities
It works through district-level health workers, ASHA workers, and local health teams.
2. National Framework for Malaria Elimination (NFME) 2016–2030
India has a clear vision to eliminate malaria by 2030.
The framework focuses on:
- Strengthening surveillance
- Treating cases quickly
- Targeting high-risk districts
- Monitoring drug resistance
- Improving diagnostic facilities
3. Malaria Elimination Demonstration Project (MEDP)
Started in Madhya Pradesh, this project showed that intense surveillance + timely treatment can reduce malaria drastically.
It serves as a model for other states.
4. Distribution of Long-Lasting Insecticidal Nets (LLINs)
Government provides treated mosquito nets to:
- Pregnant women
- Children
- Tribal and rural populations
- High-transmission areas
These nets give long-term protection, especially at night.
5. Indoor Residual Spraying (IRS)
Health workers spray insecticides on indoor walls.
Mosquitoes rest on these walls after biting, so spraying helps kill them and break the transmission cycle.
6. Regular Blood Testing and Surveillance
ASHA workers and health teams conduct door-to-door visits in high-risk areas.
They test people with fever using:
- Rapid diagnostic tests
- Microscopy
Quick treatment prevents outbreaks.
7. Public Awareness and Education Campaigns
These campaigns teach people:
- How malaria spreads
- How to prevent mosquito breeding
- Importance of early testing
- When to seek medical help
Awareness is one of the strongest tools for malaria control.
Why These Programs Matter
- Reduce malaria burden
- Protect vulnerable communities
- Prevent outbreaks
- Save lives through early diagnosis and treatment
- Support India’s goal of becoming a malaria-free nation by 2030
Myths vs. Facts About Malaria
Many people still believe old or incorrect ideas about malaria. These myths can delay treatment, increase fear, or make prevention less effective. Clearing them helps readers stay safe and make informed decisions.
Myth 1: “Malaria spreads from person to person.”
Fact: Malaria doesn’t spread through touching, sharing food, or being near someone.
It spreads only through bites of infected female Anopheles mosquitoes.
Myth 2: “Malaria only happens during the rainy season.”
Fact: Risk is higher during rains, but malaria can occur anytime mosquitoes breed — even in winter or post-monsoon.
Myth 3: “If fever goes away after a tablet, it’s not malaria.”
Fact: Fever may drop temporarily, but malaria can still be present.
Only a blood test can confirm whether malaria is gone.
Myth 4: “Sleeping in AC rooms prevents malaria.”
Fact: It lowers risk but doesn’t guarantee protection.
Mosquitoes can still enter the room or bite before bedtime.
Myth 5: “Herbal drinks or home remedies can cure malaria.”
Fact: Home remedies may relieve discomfort, but they cannot kill the malaria parasite.
Only proper antimalarial medicines can cure malaria.
Myth 6: “Vivax malaria is always mild.”
Fact: P. vivax is usually less severe than falciparum, but it can still cause:
- Severe anemia
- Jaundice
- Repeated relapses
Ignoring it is dangerous.
Myth 7: “Once you get malaria, you’ll never get it again.”
Fact: Immunity from malaria is temporary and incomplete.
A person can be infected multiple times, especially in high-risk areas.
Myth 8: “Mosquito coils and sprays are enough to prevent malaria.”
Fact: They help, but complete protection needs:
- Nets
- Repellents
- Clean surroundings
- Community measures
Why This Helps Readers
- Removes fear
- Reduces wrong beliefs
- Promotes early testing
- Encourages scientific prevention
- Helps families make safer choices
When to Seek Medical Help
One of the biggest challenges with malaria is that early symptoms look just like a normal viral fever. Many people wait too long, hoping it will go away on its own.
But getting medical help at the right time can prevent serious complications and even save lives.
Seek Medical Help If You Have These Symptoms
1. Fever With Chills That Comes and Goes
A repeating fever pattern — especially every 24 or 48 hours — is a classic sign of malaria.
2. Persistent High Fever for More Than 1–2 Days
If fever continues despite home remedies, testing is needed.
3. Severe Body Pain, Headache, or Extreme Weakness
These are early indicators the parasite is multiplying quickly.
Urgent Medical Care Needed for These Red-Flag Symptoms
These signs suggest severe malaria, which can become life-threatening:
- Confusion, drowsiness, or difficulty staying awake
- Breathing difficulty
- Seizures
- Very high fever that doesn’t respond to medicines
- Severe vomiting or inability to drink fluids
- Yellow eyes/skin (jaundice)
- Dark or very little urine
- Bleeding or bruising easily
If any of these appear, the person should go to a hospital immediately.
Special Groups That Must Seek Help Early
- Children under 5
- Pregnant women
- Elderly adults
- People with chronic illnesses
- Individuals in malaria-prone areas
They should get tested at the first sign of fever.
Why Prompt Medical Help Matters
- Prevents severe complications
- Ensures correct diagnosis (malaria test)
- Helps start treatment early
- Protects the family and community
- Improves survival and speeds up recovery
Conclusion
Malaria is still a major health challenge, but it’s also a disease we can prevent, detect early, and treat effectively. When readers understand how it spreads, what symptoms to watch for, and when to seek help, they feel more in control and less afraid.
The message is simple but powerful:
Awareness saves lives.
By using mosquito nets, avoiding stagnant water, staying alert to fever patterns, and getting tested early, families can protect themselves and their communities. The government’s programs, health workers, and diagnostic tools are all in place — people just need to use them at the right time.
Malaria may start silently, with a simple fever, but it doesn’t have to become dangerous. With the right knowledge and quick action, anyone can fight it and recover fully.