Introduction
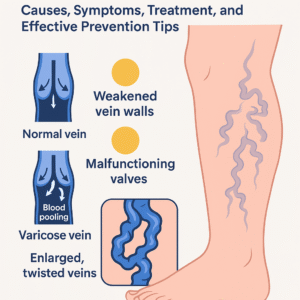
Varicose veins are swollen, enlarged, and twisted veins that usually appear on the legs. They happen when the veins in your legs struggle to push blood back up toward the heart. Because of this, blood collects inside the vein, causing it to bulge and become visible on the surface of the skin.
This condition is very common, especially in people who stand for long hours, women during pregnancy, and older adults. While varicose veins are usually not dangerous, they can cause pain, discomfort, heaviness, and cosmetic concerns. Early understanding and treatment can help prevent complications later.
Causes of Varicose Veins
Varicose veins develop when the veins in the legs cannot push blood back to the heart efficiently. This leads to blood pooling, increased pressure, and swollen, twisted veins. The major causes include:
1. Weak or Damaged Valves
Leg veins have one-way valves that keep blood moving upward.
When these valves become weak or damaged, blood flows backward and collects inside the vein, making it enlarged.
2. Genetics (Family History)
Varicose veins often run in families.
If your parents or relatives have it, there’s a higher chance you may develop it due to inherited weak vein walls or valves.
3. Prolonged Standing or Sitting
Jobs or routines that require long hours of standing or sitting reduce blood circulation.
This increases pressure in leg veins and leads to varicose veins.
4. Obesity
Excess body weight puts extra pressure on the veins.
This makes it harder for blood to flow upward, causing veins to stretch and swell.
5. Pregnancy
During pregnancy:
- Blood volume increases
- Hormonal changes relax vein walls
- The growing uterus presses on leg veins
These changes collectively increase the risk of varicose veins.
6. Hormonal Changes
Hormones like estrogen and progesterone can weaken vein walls.
This is why varicose veins are more common in:
- Women
- Pregnancy
- Menopause
- Those taking hormonal medications
7. Increasing Age
As we age, veins naturally lose elasticity.
Valves also weaken over time, making it easier for blood to flow backward and pool in the legs.
Symptoms of Varicose Veins
Varicose veins don’t just change the way your legs look — they can also create discomfort that affects daily activities. Here are the key symptoms people commonly notice:
1. Visible Swollen Veins
The most noticeable sign is enlarged, twisted, bulging veins.
They often look blue, dark purple, or rope-like, especially on the legs or calves.
2. Heaviness in the Legs
Many people feel a heavy, tired, or dragging sensation in their legs, especially after standing for long periods.
3. Pain or Aching
A dull ache or throbbing pain may develop, which may worsen:
- At the end of the day
- After long standing
- During hot weather
4. Swelling (Edema)
Ankles or lower legs may become swollen because blood isn’t returning properly to the heart.
5. Muscle Cramps
Night-time leg cramps are common due to poor blood flow.
6. Burning or Throbbing Sensation
Some people feel warmth, burning, or a throbbing feeling around the enlarged veins.
7. Itching Around the Veins
The skin around varicose veins can feel dry, itchy, or irritated — a condition called venous eczema.
8. Skin Discoloration
In advanced cases, the skin may turn:
- Brown
- Dark
- Patchy
This happens due to long-term pressure and inflammation.
9. Ulcers (Severe Cases)
If untreated, varicose veins can lead to non-healing sores near the ankles, known as venous ulcers.
Diagnosis of Varicose Veins
Diagnosing varicose veins is usually straightforward. Doctors use a combination of physical examination and tests to assess blood flow and check for complications.
1. Physical Examination
The doctor begins by:
- Looking at your legs while you’re standing or sitting
- Checking for visible swollen or twisted veins
- Asking about symptoms like pain, heaviness, swelling, or itching
This basic examination helps identify how severe the condition is.
2. Medical History
You may be asked about:
- Family history of varicose veins
- Previous blood clots
- Pregnancy history
- Lifestyle or job habits (e.g., long standing/sitting)
This helps understand your risk factors.
3. Doppler Ultrasound
This is the main diagnostic test for varicose veins.
It uses sound waves to:
- Check blood flow in the veins
- Identify valve damage
- Detect blockages or blood clots
- Assess the severity of venous reflux (backward blood flow)
It is painless, safe, and non-invasive.
4. Duplex Ultrasound
A more detailed version of Doppler ultrasound.
It provides:
- Images of the vein
- Real-time blood flow tracking
This is useful for planning treatments like laser therapy or surgery.
Treatment of Varicose Veins
Treatment depends on how severe the veins are and what symptoms the patient has. The goal is to reduce discomfort, improve appearance, and prevent complications. Treatments range from simple lifestyle changes to advanced medical procedures.
1. Lifestyle Modifications
These are the first steps and help improve blood flow:
• Regular Exercise
Walking, cycling, and leg-strengthening exercises help the calf muscles pump blood upward.
• Weight Management
Reducing excess weight lowers pressure on the leg veins.
• Avoid Long Standing or Sitting
Taking short breaks to stretch or walk improves circulation.
• Leg Elevation
Keeping legs raised above heart level reduces swelling.
2. Compression Stockings
These are specially designed elastic stockings that:
- Apply gentle pressure
- Improve blood flow
- Reduce swelling and pain
They are a safe, non-invasive option and commonly recommended.
3. Medications
Although no medicine can “cure” varicose veins, some drugs help:
- Reduce swelling
- Improve vein tone
- Relieve pain and heaviness
Often used for supportive care.
4. Sclerotherapy
A doctor injects a special solution into the vein, causing it to:
- Collapse
- Seal shut
- Gradually fade over weeks
Effective for small and medium-sized varicose or spider veins.
5. Laser Treatment (EVLT – Endovenous Laser Therapy)
A laser fiber is inserted into the vein to heat and close it.
Benefits include:
- Minimally invasive
- Quick recovery
- Less pain
- High success rate
6. Radiofrequency Ablation (RFA)
Similar to laser treatment but uses radiofrequency energy to close the vein.
It is safe, effective, and often preferred for larger veins.
7. Microphlebectomy (Ambulatory Phlebectomy)
Small incisions are made to remove surface varicose veins.
It is a minor procedure with minimal scarring.
8. Vein Stripping (Rarely Used Now)
A surgical method to remove large, damaged veins.
Used only when other treatments are not suitable.
Home Remedies for Varicose Veins
These home remedies don’t cure varicose veins, but they reduce symptoms, improve blood flow, and help prevent the condition from worsening. They’re safe, easy, and effective for daily use.
1. Leg Elevation
Raising your legs above heart level helps:
- Reduce swelling
- Improve blood circulation
- Decrease heaviness
Do this for 15–20 minutes, 2–3 times a day.
2. Regular Exercise
Gentle exercises boost blood flow and strengthen leg muscles.
Helpful exercises include:
- Walking
- Cycling
- Swimming
- Calf raises
Movement prevents blood from pooling in the legs.
3. Massage the Legs
Light massage improves circulation and reduces discomfort.
Use upward strokes — but avoid pressing directly on swollen veins.
4. Warm Water Baths
A warm bath relaxes the veins and improves blood flow.
Avoid very hot water as it may worsen swelling.
5. Compression Stockings (Daily Use)
Wearing compression stockings helps:
- Reduce pain
- Control swelling
- Improve circulation
They are one of the most effective home-care options.
6. Avoid Tight Clothing
Tight clothes around the waist or legs restrict blood flow.
Choose loose, comfortable clothing.
7. Stay Hydrated
Proper water intake keeps the blood thinner and helps prevent swelling.
8. Diet Rich in Fiber & Antioxidants
Fiber prevents constipation, which reduces pressure on leg veins.
Antioxidants strengthen vein walls.
Helpful foods:
- Fruits
- Vegetables
- Whole grains
- Nuts
- Seeds
9. Avoid Long Sitting or Standing
Take short breaks every 30–45 minutes.
Move your legs, stretch, walk — anything to keep blood flowing.
When to See a Doctor
Most varicose veins are harmless, but some signs mean the condition is getting worse and needs medical attention. Seeing a doctor at the right time helps prevent serious complications.
1. Persistent Pain or Discomfort
If your legs feel constantly heavy, painful, throbbing, or aching, even after rest or home remedies, it’s time to consult a doctor.
2. Swelling That Doesn’t Improve
Continuous swelling of the legs or ankles — especially if it gets worse by evening — can indicate poor circulation or venous insufficiency.
3. Skin Changes
Seek medical help if you notice:
- Darkening of the skin
- Hard, thickened patches
- Red, irritated skin
These are signs of advanced vein disease.
4. Open Sores or Ulcers
If you develop wounds near the ankles that don’t heal, it could be a venous ulcer — a serious complication that requires treatment.
5. Sudden Bleeding
If a varicose vein bursts and bleeds, even slightly, it needs urgent medical assessment.
6. Sudden Increase in Pain or Swelling
This could indicate a blood clot, especially if the leg feels warm, red, or tender.
7. If the Veins Are Rapidly Getting Worse
More veins appearing quickly, or existing veins becoming large and painful, is a sign to seek expert care.
8. Cosmetic Concerns
If varicose veins affect confidence, comfort, or quality of life, professional treatments can help safely improve appearance.
Conclusion
Varicose veins are common, and for many people, they’re more than just a cosmetic concern. They can cause discomfort, heaviness, and long-term skin changes if ignored. The good news is that early recognition, simple lifestyle changes, and timely medical care can significantly improve symptoms and prevent complications.
By staying active, maintaining a healthy weight, avoiding long hours of standing or sitting, and using compression stockings when needed, most people can manage varicose veins effectively. And whenever pain, swelling, skin changes, or ulcers appear, seeking medical advice is the safest step.
Caring for your vein health isn’t just about appearance — it’s about comfort, mobility, and long-term wellness. With the right approach, varicose veins can be well controlled, allowing you to stay active and confident.