Introduction
The nursing process is the backbone of professional nursing practice. It gives nurses a structured, scientific, and patient-centered way to provide care.
Instead of working randomly, the nursing process helps nurses think clearly, plan properly, and care for each patient in a systematic manner.
It ensures that:
- Every patient receives individualized care, not general care
- Nursing actions are organized and purposeful
- Care is based on assessment, evidence, and evaluation
In simple words, this introduction sets the stage by showing that the nursing process isn’t just a theory—it’s the real, day-to-day method nurses use to improve patient outcomes and maintain safety.
What is the Nursing Process?
The nursing process is a systematic, scientific, and organized approach used by nurses to identify patient needs, plan care, provide interventions, and evaluate outcomes.
It acts like a clinical roadmap that guides nurses at every step of patient care.
Key things to understand:
- It is problem-solving in nature — nurses collect information, analyse it, and decide what to do next.
- It helps deliver safe, effective, and personalized care rather than one-size-fits-all treatment.
- It connects assessment → diagnosis → planning → implementation → evaluation in a continuous cycle.
- It improves communication within the healthcare team because everyone follows the same structured method.
In short, the nursing process ensures that nursing care is organized, evidence-based, and focused on each patient’s unique condition.
Key Characteristics of the Nursing Process
The nursing process has several unique features that make it reliable and effective in real clinical practice. These characteristics ensure that care is organized, flexible, and centered around the patient.
1. Systematic
Nurses follow a step-by-step method.
Nothing is random — each step flows logically from assessment to evaluation.
This reduces errors and ensures complete, accurate care.
2. Evidence-Based
Decisions are made using scientific knowledge, clinical experience, and research.
It prevents guessing and promotes safe, high-quality care.
3. Patient-Centered
The focus is always on individual patient needs, preferences, and values.
Every care plan is tailored so the patient receives what they specifically require.
4. Dynamic and Cyclical
The nursing process is not rigid.
Nurses continuously reassess, update, and adjust the care plan as the patient’s condition changes.
5. Goal-Oriented
Each intervention aims toward clear, measurable goals that improve patient health.
This makes nursing care purposeful and results-focused.
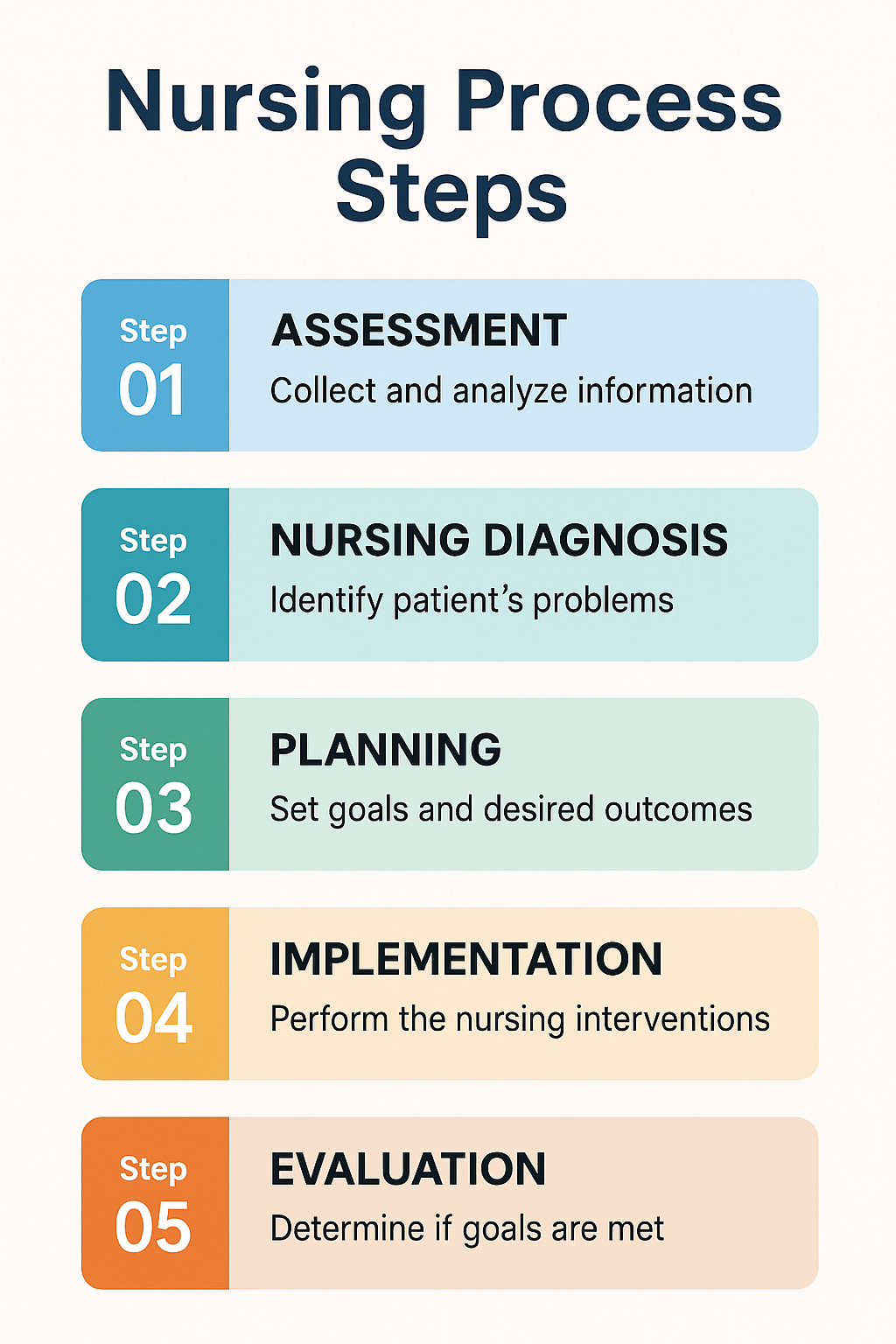
Step 1 – Assessment
Assessment is the first and most important step of the nursing process.
Here, the nurse collects complete, accurate, and relevant information about the patient’s health status.
Why Assessment Matters
A good assessment is the foundation of correct diagnosis and effective care.
If assessment is wrong or incomplete, the entire care plan becomes weak.
Types of Data Collected
- Subjective Data:
Information the patient tells the nurse
(e.g., pain level, nausea, dizziness, fatigue). - Objective Data:
Information the nurse observes or measures
(e.g., BP, temperature, lab reports, physical signs).
Methods Used in Assessment
- Observation: Noticing patient behavior, appearance, distress.
- Physical Examination: Inspection, palpation, percussion, auscultation.
- Interviewing: Asking structured or open-ended questions.
- Review of Records: Medical history, lab reports, previous notes.
Goal of Assessment
To create a complete picture of the patient’s physical, emotional, psychological, and social condition.
Step 2 – Nursing Diagnosis
After collecting all assessment data, the nurse moves to the nursing diagnosis stage.
This step helps identify the patient’s actual health problems, potential risks, or wellness needs.
What is a Nursing Diagnosis?
A nursing diagnosis is a clinical judgment made by the nurse about the patient’s response to health conditions or life processes.
It focuses on how the patient is affected — not on the disease itself.
Nursing Diagnosis vs Medical Diagnosis
- Medical Diagnosis:
Identifies a disease (e.g., pneumonia, diabetes). - Nursing Diagnosis:
Identifies the patient’s response to that disease
(e.g., ineffective airway clearance, risk for infection, impaired mobility).
Types of Nursing Diagnoses
- Actual Diagnosis – the problem exists now
- Risk Diagnosis – the patient is vulnerable to a problem
- Wellness Diagnosis – for improving or promoting health
Why This Step Is Important
- Helps nurses plan the right interventions
- Ensures care is individualized and focused
- Improves patient safety and outcomes
Examples
- Acute pain related to surgical incision
- Risk for falls related to weak muscles
- Impaired skin integrity related to immobility
Step 3 – Planning
Once the nursing diagnosis is identified, the next step is planning.
Here, the nurse creates a structured care plan with clear goals and specific interventions tailored to the patient’s needs.
Purpose of Planning
To decide what needs to be achieved, how it will be achieved, and within what time frame.
Good planning ensures care is organized, measurable, and focused.
Key Components of Planning
1. Setting Goals and Expected Outcomes
Nurses use SMART goals:
- Specific
- Measurable
- Achievable
- Realistic
- Time-bound
Example:
“Patient will maintain oxygen saturation above 95% within 24 hours.”
2. Prioritizing Patient Problems
Some problems are more urgent than others.
Nurses prioritize based on:
- Severity
- Safety needs
- Life-threatening conditions
- Maslow’s hierarchy
3. Selecting Nursing Interventions
These are the actions the nurse will take to achieve the goals.
They may include:
- Monitoring
- Teaching
- Direct care
- Preventive measures
- Coordination with other healthcare professionals
Outcome of the Planning Step
A care plan that guides all future nursing actions, ensuring the patient receives well-organized, evidence-based care.
Step 4 – Implementation
Implementation is the action stage of the nursing process.
Here, the nurse puts the care plan into action by carrying out the interventions that were planned in the previous step.
What Happens in Implementation?
Nurses provide direct and indirect care to help the patient meet the set goals.
Types of Nursing Interventions
1. Direct Care Interventions
These involve hands-on care, such as:
- Administering medications
- Wound dressing
- Assisting with mobility
- Monitoring vital signs
- Providing hygiene care
2. Indirect Care Interventions
These support patient care but are not done directly to the patient:
- Documentation
- Communicating with healthcare team
- Coordinating referrals
- Maintaining infection control practices
Important Tasks During Implementation
- Following the care plan accurately
- Observing the patient’s response
- Teaching the patient and family
- Ensuring safety and comfort
- Updating records to maintain continuity of care
Why Implementation Matters
This step turns the plan into action and ensures the patient receives timely, appropriate, and evidence-based nursing care.
Step 5 – Evaluation
Evaluation is the final step of the nursing process.
Here, the nurse checks whether the planned goals and outcomes have been achieved or not.
What Evaluation Involves
- Reviewing the patient’s current condition
- Comparing actual outcomes with expected outcomes
- Checking if the patient’s problems have improved, resolved, or worsened
Types of Evaluation Outcomes
1. Goal Met
The patient achieved the desired outcome.
Example: Pain level reduced from 7/10 to 2/10.
2. Goal Partially Met
Some improvement is seen, but the full goal isn’t achieved.
Example: Mobility improved but still limited.
3. Goal Not Met
No progress or patient condition worsened.
Example: Wound not healing as expected.
Actions After Evaluation
- If goals are met → Continue or discontinue plan
- If goals are partially met/not met → Modify the care plan
- Reassess the patient
- Change interventions
- Set new goals
Why Evaluation is Important
- Ensures that nursing care is effective and meaningful
- Helps identify what is working and what needs change
- Promotes continuous improvement in patient care
Importance of the Nursing Process
The nursing process is important because it brings clarity, safety, and structure to patient care.
It ensures that nursing care is scientific, systematic, and centered on the patient’s real needs.
Why the Nursing Process Is Important
1. Ensures Quality Care
The step-by-step method helps nurses provide accurate, efficient, and holistic care.
2. Improves Critical Thinking
Nurses analyze data, make judgments, and think logically.
This strengthens professional decision-making skills.
3. Promotes Patient Safety
By following structured steps, nurses reduce errors and identify risks earlier.
4. Enhances Communication
Each step involves documentation and teamwork.
It helps the entire healthcare team stay coordinated and consistent.
5. Provides Individualized Care
Every plan is tailored to the patient’s specific needs, preferences, and condition.
6. Supports Evidence-Based Practice
Interventions are chosen based on research, guidelines, and clinical knowledge.
7. Helps Evaluate Progress
Nurses can measure what is working and what is not, leading to continuous improvement.
Advantages of the Nursing Process
The nursing process offers many practical benefits that improve both patient care and nursing efficiency.
It gives nurses a clear framework to deliver safe, high-quality, and organized care.
Major Advantages
1. Provides a Clear Structure
Nurses know exactly what to do at each step — from assessment to evaluation.
This avoids confusion and improves decision-making.
2. Enhances Continuity of Care
Because everything is documented and structured, any nurse can continue care smoothly even during shifts.
3. Improves Patient Outcomes
Focused assessment, accurate diagnosis, and evidence-based interventions lead to better recovery and health results.
4. Individualizes the Care Plan
Each patient gets a unique plan designed specifically for their needs — not a generalized routine.
5. Increases Patient Satisfaction
When care is organized and responsive to patient needs, patients feel heard, supported, and cared for.
6. Supports Professional Growth
Nurses develop stronger skills in:
- Critical thinking
- Observation
- Communication
- Clinical judgment
7. Encourages Evidence-Based Practice
Interventions are chosen based on research and proven guidelines, making care safer and more reliable.
Challenges in Implementing the Nursing Process
Even though the nursing process is highly effective, nurses often face practical challenges while applying it in real clinical settings.
These challenges can affect the quality and speed of patient care.
Major Challenges
1. Time Constraints
Hospitals are busy, workloads are high, and nurses often have many patients.
Because of this, completing all steps of the nursing process can feel rushed.
2. Heavy Workload
Short staffing, emergencies, and multiple responsibilities make it difficult to perform detailed assessments and documentation.
3. Lack of Training or Experience
Some nurses, especially beginners, may struggle with writing proper nursing diagnoses or planning SMART goals.
4. Documentation Burden
The process requires accurate documentation, which can be time-consuming and overwhelming during busy shifts.
5. Patient Complexity
Patients with multiple diseases or chronic conditions need more detailed assessment and planning, which takes more time and skill.
6. Limited Resources
Shortage of equipment, support staff, or educational tools can make implementation harder.
7. Poor Communication
If communication within the healthcare team is weak, planning and implementation become less effective.
Practical Tips for Nurses
These practical tips help nurses apply the nursing process more effectively in real clinical situations.
They make assessments faster, diagnoses more accurate, and interventions more meaningful.
Useful and Actionable Tips
1. Perform Focused Assessments
Instead of collecting everything, focus on what is most relevant to the patient’s condition.
This saves time and improves accuracy.
2. Use Standard Nursing Languages (NANDA, NIC, NOC)
These help create clear diagnoses, select suitable interventions, and evaluate outcomes properly.
3. Prioritize Patient Problems
Use critical thinking to decide what is:
- Urgent
- Safety-related
- Most important for the patient’s recovery
4. Communicate with Patients and Families
Ask questions, listen actively, and explain the care plan.
This builds trust and improves outcomes.
5. Collaborate with Healthcare Team
Working together with doctors, physiotherapists, dietitians, and others ensures consistent, coordinated care.
6. Document Everything Properly
Accurate records help with continuity of care and legal safety.
7. Keep Updating Knowledge
Nursing guidelines change over time.
Learning new skills and techniques improves the quality of care.
8. Stay Organized During Implementation
Prepare equipment early, plan your workflow, and follow a routine to save time during a busy shift.
Clinical Example of the Nursing Process
A simple, real-life example helps students understand how the nursing process works from start to finish.
This example shows how each step connects logically.
Case Scenario
A 60-year-old patient is admitted with shortness of breath, cough, and fatigue.
Step-by-Step Application
1. Assessment
- Subjective data:
Patient says, “I feel breathless even while resting.” - Objective data:
RR 28/min, SpO₂ 88%, wheezing on auscultation, high temperature.
2. Nursing Diagnosis
- Impaired gas exchange related to airway inflammation
- Ineffective breathing pattern related to respiratory distress
3. Planning
Set SMART goals:
- Patient will maintain SpO₂ above 94% within 24 hours.
- Patient’s respiratory rate will reduce to 20–24/min.
Select interventions:
- Monitor SpO₂ and RR every 2 hours
- Elevate head of the bed
- Administer oxygen as prescribed
- Encourage deep breathing exercises
4. Implementation
Carry out the plan:
- Provide oxygen
- Position the patient upright
- Monitor vitals
- Teach breathing techniques
- Record all findings clearly
5. Evaluation
- SpO₂ improved to 95%
- RR decreased to 22/min
- Patient reports easier breathing
Goal met → Continue with supportive care.
Conclusion
The nursing process is much more than a theoretical framework — it is the heart of professional nursing practice.
By following its five systematic steps, nurses deliver care that is organized, safe, and patient-centered.
It helps nurses:
- Think critically
- Make accurate decisions
- Provide individualized care
- Evaluate progress and improve outcomes
In a healthcare environment that is constantly changing, the nursing process ensures that every patient receives holistic, evidence-based, and compassionate care.
When applied consistently, it strengthens the nurse–patient relationship and leads to better recovery, comfort, and trust.