Introduction to Piles (Hemorrhoids)
Piles, also known as hemorrhoids, are swollen veins in and around the rectum or anus. They’re very common, and almost every person experiences them at least once in life. Even though the condition can feel embarrassing or uncomfortable to talk about, it’s important to know that piles are not dangerous and are usually easy to manage with proper care.
Many people develop piles because of constipation, long sitting hours, low-fiber diets, pregnancy, or even stress. The good news is that most cases improve with simple lifestyle changes, good toilet habits, and timely treatment.
Types of Piles
Piles are mainly divided into two types, based on where the swollen veins develop. Understanding the difference helps you to identify their symptoms better and seek the right treatment.
a) Internal Piles
These develop inside the rectum, so they’re usually not visible from outside.
Because there are fewer pain-sensing nerves inside the rectum, internal piles typically don’t cause pain, but they may lead to:
- Painless bleeding during bowel movements
- Mucus discharge
- A sensation of incomplete evacuation
Internal piles are often noticed only when bleeding occurs.
b) External Piles
These form under the skin around the anus, where nerves are highly sensitive. That’s why external piles often cause:
- Pain and discomfort
- Swelling or a painful lump
- Itching or irritation
- Sometimes blood clots, making the pain sharper
External piles are usually easier to notice because they are visible and more symptomatic.
Common Causes of Piles
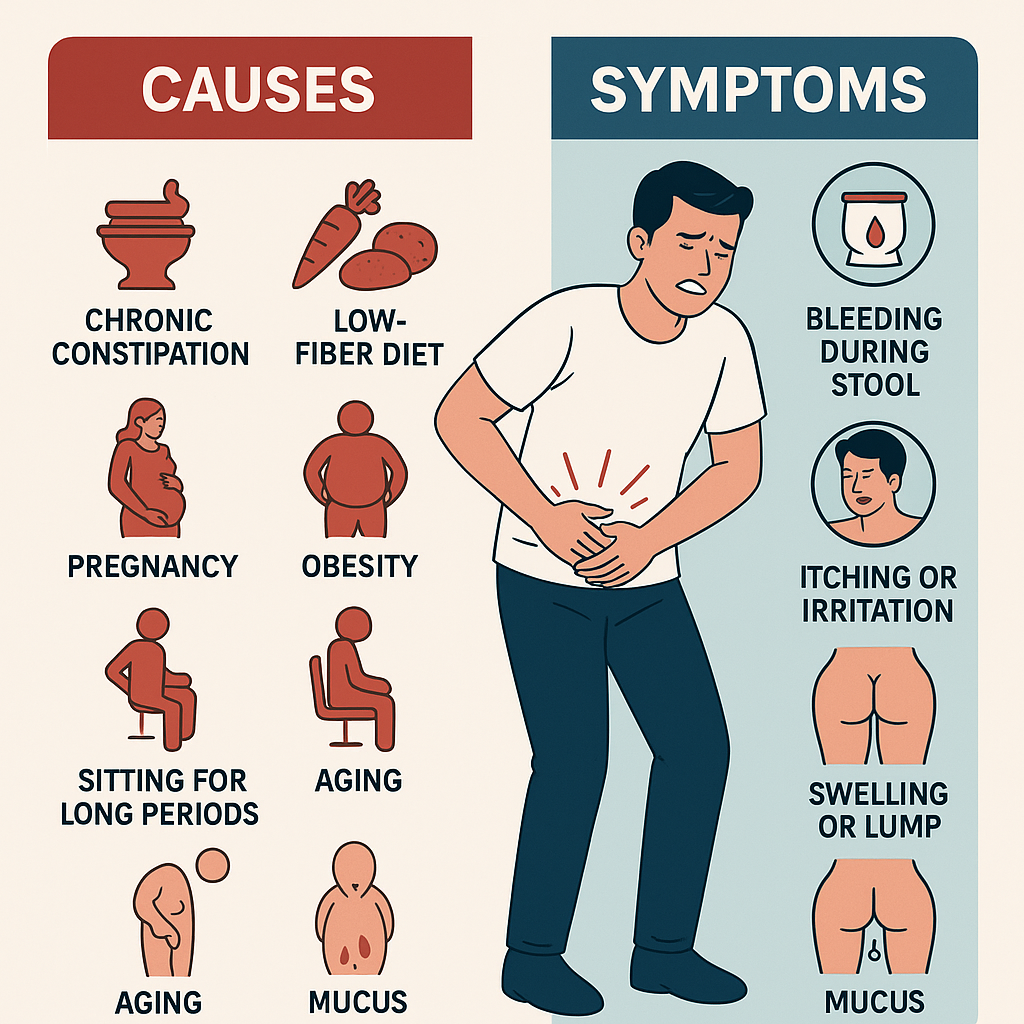
Piles usually develop because of increased pressure on the veins in the rectum and anus. This pressure makes the veins swell, leading to discomfort, pain, or bleeding. The most common causes include:
a) Chronic Constipation
Straining too hard while passing stool puts direct pressure on the veins. Over time, this repeated strain can cause piles.
b) Low-Fiber Diet
When the diet lacks fiber, stools become hard and difficult to pass. This leads to straining during bowel movements.
c) Pregnancy
Growing uterus, hormonal changes, and increased abdominal pressure make piles more common in pregnant women.
d) Obesity
Excess body weight increases pressure on the pelvic region, contributing to swollen veins.
e) Sitting for Long Periods
Sitting for long hours—especially on the toilet—reduces blood flow and increases pressure around the anus.
f) Aging
As we age, the tissues supporting veins in the rectum weaken, making piles more likely.
g) Heavy Lifting
Repeated lifting of heavy objects can trigger straining and increase pressure in the lower body.
Symptoms of Piles
Piles can show up with different symptoms depending on whether they’re internal or external. Knowing these signs early helps people manage the condition before it becomes severe.
a) Bleeding During Stool
The most common symptom. You may notice bright red blood on the toilet paper or in the toilet bowl.
b) Pain or Discomfort
External piles especially cause sharp or aching pain, especially while sitting or passing stool.
c) Itching or Irritation
Swelling around the anus can lead to constant itchiness, making the skin more sensitive.
d) Swelling or a Lump
A small lump or swelling near the anus is common in external piles. It may be painful or tender to touch.
e) Mucus Discharge
Internal piles can sometimes cause mucus leakage, leading to irritation and discomfort.
f) Feeling of Incomplete Evacuation
People often feel like the bowel didn’t fully empty, even after passing stool.
Risk Factors for Piles
Some people are more likely to develop piles because of certain lifestyle habits, body conditions, or daily routines. These risk factors don’t always cause piles directly, but they increase the chances of the problem occurring.
a) Sedentary Lifestyle
Sitting for long hours—especially without breaks—reduces blood flow to the lower body and puts pressure on rectal veins.
b) Low-Fiber Eating Habits
Regularly eating food low in fiber leads to hard stools, which increases the risk of straining and developing piles.
c) Dehydration
Not drinking enough water causes the stool to become dry and difficult to pass.
d) Family History
If close family members have piles, the chances may be slightly higher due to genetics and similar lifestyle habits.
e) Obesity
Excess body weight increases pressure on pelvic veins, making them more likely to swell.
Diagnosis of Piles
Diagnosing piles is usually simple and quick. Doctors use a combination of physical examination and, if needed, internal inspection to confirm the condition. The process is usually painless and helps rule out other causes of bleeding or discomfort.
a) Physical Examination
For external piles, the doctor gently checks the area around the anus.
- Swelling
- Lumps
- Tender areas
These signs help identify external hemorrhoids immediately.
b) Digital Rectal Examination (DRE)
For internal piles, the doctor inserts a gloved, lubricated finger into the rectum to feel for abnormalities.
This helps check:
- Internal swelling
- Tender veins
- Any unusual growths that need further evaluation
It’s brief and generally not painful, just mildly uncomfortable.
c) Anoscopy
If deeper inspection is needed, the doctor may use an anoscope, a small tube with light.
This allows them to:
- Clearly view internal piles
- Identify the exact grade
- Plan proper treatment
Anoscopy is helpful for spotting early-stage internal hemorrhoids that don’t show symptoms clearly.
Treatment Options for Piles
Treatment for piles depends on how severe the symptoms are. Most people get relief with simple home remedies, but some may need medications or medical procedures. Here’s a breakdown:
a) Home Remedies
These are usually the first line of treatment and work well for mild to moderate piles.
- Increase fiber intake (fruits, vegetables, whole grains) to soften stool.
- Drink plenty of water to reduce constipation.
- Warm sitz bath: Sitting in warm water for 10–15 minutes helps reduce pain and swelling.
- Avoid straining during bowel movements.
- Regular exercise improves digestion and reduces pressure on veins.
b) Medications
Doctors may recommend:
- Ointments and creams to reduce pain, itching, and swelling.
- Suppositories for internal piles.
- Stool softeners or mild laxatives to make bowel movements easier.
- Pain relievers in case of discomfort.
These medicines help control symptoms while the underlying cause (like constipation) is treated.
c) Medical Procedures
If piles don’t improve with home care or medicines, minor procedures may be needed.
- Rubber Band Ligation: A rubber band is placed around the base of the pile to cut off blood supply, causing it to shrink.
- Sclerotherapy: A chemical solution is injected to shrink the piles.
- Infrared Coagulation: Heat is used to seal swollen veins.
- Hemorrhoidectomy: Surgical removal, used only in severe or recurring cases.
These procedures are usually quick, safe, and effective.
Diet for Managing Piles
A proper diet plays a major role in reducing symptoms, preventing constipation, and speeding recovery from piles. The goal is to keep stools soft and easy to pass, so there’s less strain on rectal veins.
a) High-Fiber Foods
Fiber adds bulk to stool and helps it move smoothly through the intestines.
Include more of:
- Fruits: papaya, banana, apples, pears
- Vegetables: spinach, broccoli, carrots
- Whole grains: oats, wheat bran, brown rice
- Legumes: beans, lentils
b) Adequate Water Intake
Water softens the stool and prevents dryness.
Try to drink 8–10 glasses of water every day.
c) Avoid Spicy and Oily Foods
These can irritate the digestive tract and worsen symptoms like burning or itching.
d) Limit Caffeine and Alcohol
Both can cause dehydration, making stools harder and bowel movements more difficult.
e) Add Natural Laxatives
Foods like prunes, figs, chia seeds, and flaxseeds help ease constipation naturally.
f) Avoid Processed Foods
Fast foods, refined flour, and packaged snacks slow down digestion and increase constipation.
Lifestyle Tips for Managing and Preventing Piles

Lifestyle changes make a big difference in reducing symptoms and preventing piles from coming back. These habits support healthy digestion, reduce pressure on veins, and improve overall bowel health.
a) Regular Exercise
Physical activity keeps the digestive system active and prevents constipation.
Even 20–30 minutes of walking daily can help reduce symptoms.
b) Avoid Sitting for Long Hours
Sitting too long—especially on hard surfaces—puts pressure on the veins around the anus.
Take short breaks every 45–60 minutes to stretch or walk.
c) Practice Healthy Toilet Habits
- Don’t hold in stools for too long.
- Avoid reading or using the phone on the toilet.
- Don’t strain while passing stool.
These simple habits prevent unnecessary pressure on rectal veins.
d) Maintain a Healthy Weight
Losing excess weight reduces abdominal pressure and lowers the risk of piles.
e) Stress Management
Stress may affect digestion and bowel habits.
Deep breathing, yoga, or even light stretching helps maintain gut health.
f) Improve Posture
Sitting with proper posture supports pelvic muscles and reduces rectal pressure.
When to See a Doctor
While most cases of piles improve with home care, it’s important to know when professional help is needed. Timely medical attention prevents complications and ensures faster relief.
a) Heavy or Continuous Bleeding
If you notice persistent bleeding during or after bowel movements, it’s best to consult a doctor.
Bleeding may also signal other conditions that need diagnosis.
b) Severe Pain or Swelling
Sharp, unbearable pain—especially with a lump—may indicate a thrombosed or strangulated hemorrhoid.
c) Symptoms Not Improving with Home Care
If lifestyle changes, diet correction, and medicines don’t work within one to two weeks, medical treatment may be needed.
d) Difficulty Passing Stool
If bowel habits change suddenly or stools become consistently painful to pass, a check-up is advisable.
e) Fever or Signs of Infection
Redness, warmth, pus, or fever along with piles symptoms can indicate an infection that needs immediate treatment.
f) Unexplained Weight Loss or Weakness
Though rare, these symptoms should not be ignored and require evaluation.
Conclusion
Piles may feel uncomfortable, painful, or even embarrassing, but the truth is it’s a very common condition that people of all ages experience. With the right awareness and early care, most cases improve easily through simple lifestyle changes, a fiber-rich diet, proper hydration, and healthy toilet habits.
If symptoms become severe or don’t improve with home treatment, seeking medical help is always a smart and safe step. Modern treatments are quick, effective, and designed to bring long-lasting relief.
The key takeaway for you is this:
listen to your body, don’t ignore symptoms, and make small daily changes that support your digestive health.